Broken fingers are common hand injuries. These injuries are also called “phalanx fractures” and they can occur from a variety of injuries such as a fall, a motor vehicle collision, or sports injury. There are fourteen phalanges in each hand — three in each finger and two in the thumb. The phalanges make up the bony architecture of the fingers and they are very important for normal hand function.
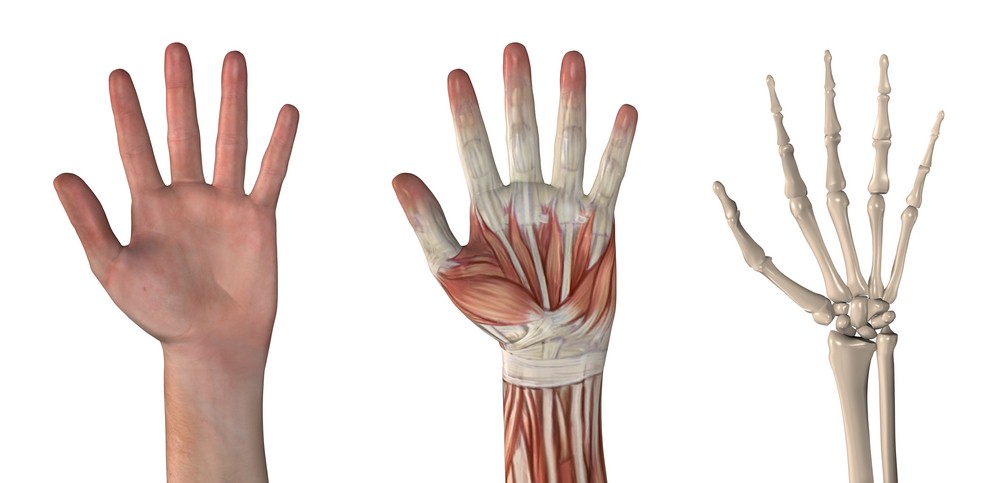
If you recently injured your finger and are wondering if it is broken, the best thing to do is get an x-ray to find out. You can get x-rays in your physician’s office, urgent care, or local emergency room. Many breaks or fractures in the fingers can be misdiagnosed as “just a sprain” or a “jammed finger.” If a finger fracture is not treated appropriately, the long-term results may not be good. I have heard from many patients “I could still move it, so I didn’t think it was broken.” While in many cases, a fracture causes the finger to be stiff and difficult to move, however, this is not true in all cases. When in doubt, get it checked out.
What are the treatment options for a broken finger?
The treatment plan is individualized, based on the x-rays and the patient’s unique needs. Satisfactory healing of the fracture is important to restore the function of the hand. Early diagnosis and treatment is very important, and hand therapy can help with range of motion, swelling, and strength during the healing process.
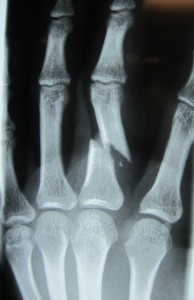
Most patients have fractures which are well-aligned, or “minimally displaced.” These patients usually do not need surgery. Treatment in these cases is typically rest and protection of the fracture with a splint for a few weeks. Sometimes “buddy-taping” to the uninjured, neighboring finger can be used in stable fractures. Follow-up x-rays are obtained to see how the fracture is healing, and to evaluate for displacement.
Some displaced fractures can be re-aligned without surgery, called “closed reduction”, and these patients can also be treated non-operatively. This procedure can be done in the office using numbing medicine (lidocaine) in many cases. Hand therapy is often helpful in improving range of motion and strength after the fracture heals.
Some patients have fractures which are more severe and the alignment of the fracture is poor. Depending on the patient’s health and activity level, surgery may be advised to improve and maintain the alignment. A fracture which heals in bad alignment (“crooked”) can affect the patient’s grip strength and hand function. Fractures which injure the joint surface are more prone to complications such as finger stiffness and arthritis.
What is involved with phalanx fracture surgery?
The surgery is performed on an outpatient basis using either local or regional anesthesia (nerve block). During the surgery I improve the alignment of the phalanx fracture and use an implant to stabilize the bones. Fluoroscopic x-rays are used in the operating room to check the alignment. In many cases I can use temporary pins to hold the bones in place. This is a minimally-invasive technique with less scaring and is called “closed reduction and percutaneous pinning”.
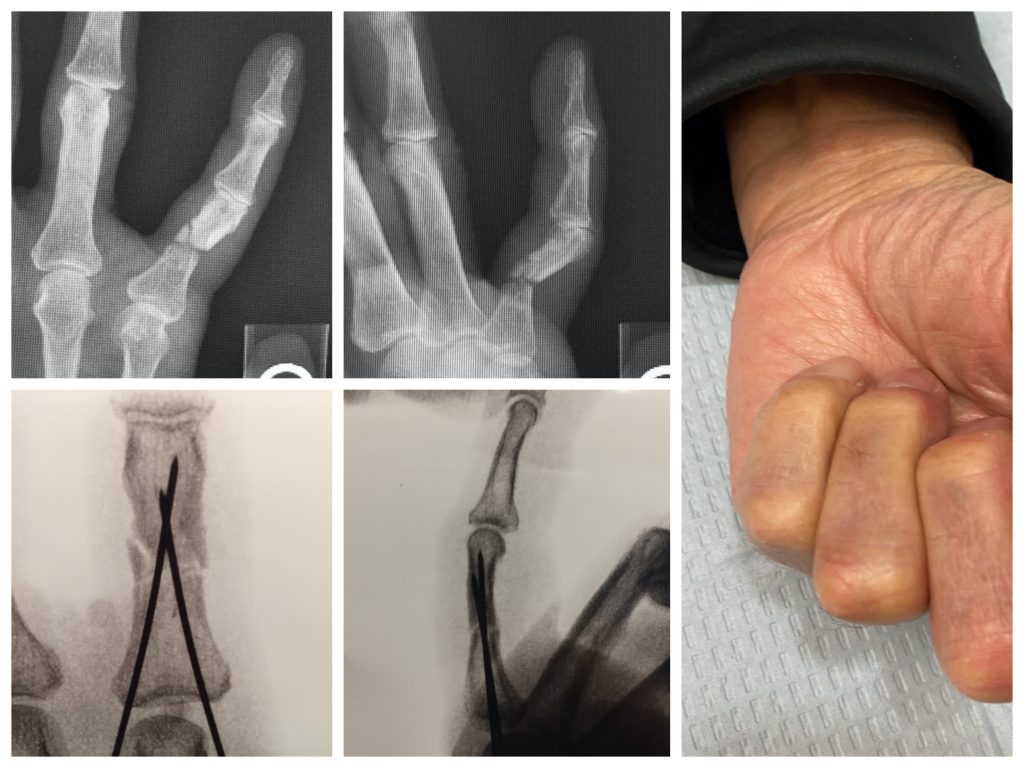
Sometimes, an incision has to be made in order to re-position the bones, and then I use a small plate and/or screws to fix the bones. This is called “open reduction and internal fixation”. Which technique is used depends on the patient and fracture pattern and is often determined in the operating room.
Surgery does not really “heal” the fracture; it simply allows the bones to be held in good alignment while the body bridges the fracture site with new bone. This healing process takes a few weeks.
Disclaimer: Please note, the material provided on this site is intended for general information only and does not constitute medical advice. This does not replace evaluation by a doctor. Please seek medical evaluation if you have a concern.
